Staying Fit
The novel coronavirus has spread across the nation at record speed, infecting millions of Americans and killing more than 150,000. Although COVID-19 attacks people of all ages, genders and ethnicities, older adults are particularly vulnerable — about 80 percent of COVID-related deaths occur among people over age 65, according to the Centers for Disease Control and Prevention (CDC).
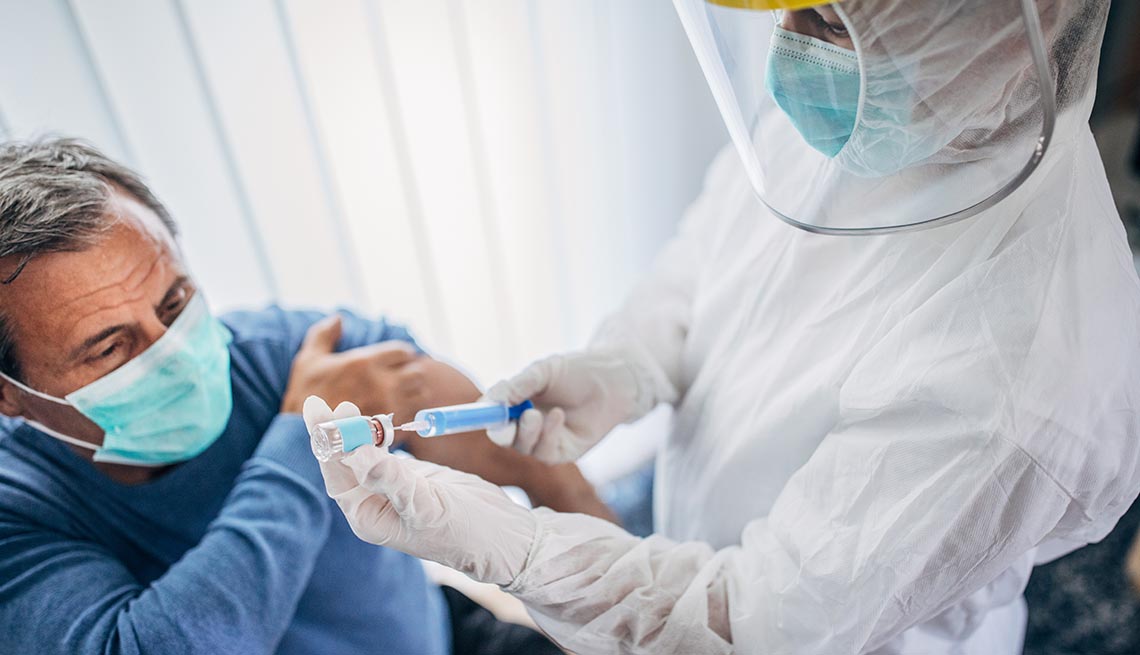
Almost two dozen vaccines are in various stages of testing around the world, with one, Moderna's mRNA-1273, already showing promising results. But most vaccines typically take anywhere from eight to 15 years to develop, test and produce. Up until now, the fastest was the mumps vaccine, which took four years. Here in the United States, the government vowed this spring to have a COVID-19 vaccine ready within 12 to 18 months and has created a project known as Operation Warp Speed, investing over $1 billion with the goal of providing enough vaccine for 300 million Americans by January.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
But with that accelerated timeline come worries that any vaccine developed will not have had enough testing — especially safety testing — behind it. History shows it pays to be cautious. Case in point: the Cutter incident of 1955, when some batches of an approved polio vaccine turned out to contain insufficiently inactivated live virus. This led to more than 250 cases of polio, many of which resulted in paralysis. More recently, the RotaShield vaccine, the first rotavirus gastroenteritis vaccine, was recalled in 1999, about a year after U.S. Food and Drug Administration (FDA) approval, after it was linked to bowel obstruction in infants.
The good news: Experts say you can feel very confident that any vaccine that makes it through FDA approval today is safe. “It is important to reassure older adults that we are not cutting corners at all,” says Mark Mulligan, M.D., director of the Division of Infectious Diseases and Immunology at the New York University Langone Health in New York City. “The speed comes from doing things in parallel that would normally done sequentially — for example, producing a vaccine at the same time as we're doing studies to make sure it's effective, safe and tolerated well."
To understand the steps researchers are taking to streamline vaccine development, it's helpful to understand a little bit more about vaccines. These are designed to mimic the immune response you develop after you're exposed to an infection. “They prime your immune system to recognize a certain virus or bacteria and to produce antibodies against it, so that the next time it shows up, your body revs up with enough force to fight it,” says William Schaffner, M.D., professor of preventive medicine, Division of Infectious Diseases, at Vanderbilt University Medical Center in Nashville. This teaches the immune system to recognize the pathogen, enabling the body to clear the infection the next time it is exposed.