Staying Fit

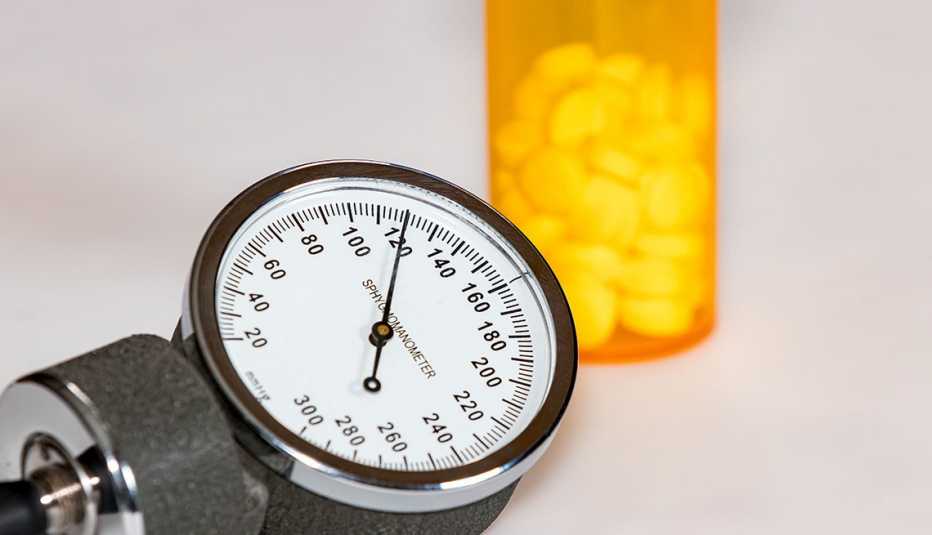
Older adults who take certain blood pressure medications could experience a slight benefit when it comes to memory, a study suggests, adding to growing evidence that blood pressure and brain health go hand in hand.
Researchers analyzed data from 14 studies of nearly 12,900 adults 50 and older with hypertension and found that those who took an angiotensin-converting-enzyme (ACE) inhibitor or an angiotensin II receptor blocker (ARB) that crossed the blood-brain barrier — a border of cells that prevents many substances in the bloodstream from entering the brain — had better memory recall across a three-year span than people who took ACE inhibitors or ARBs that stayed in the bloodstream. Eight blood pressure medications in all were identified as potentially benefiting memory. The findings were published in the journal Hypertension in June 2021.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
Exploring benefits beyond blood pressure control
High blood pressure is a risk factor for cognitive decline and dementia, and research shows that lowering it can help curb those risks. Most notably, a large federally funded trial found that intensively treating high blood pressure reduced cases of mild cognitive impairment, a precursor to dementia, by 19 percent.
Whether certain blood pressure medications come with added benefits for the brain is still in question. But this recent study “gets us one step closer to better understanding” the relationship between blood pressure and brain health and the potential influence medications may have, says Dave Dixon, professor of pharmacy at Virginia Commonwealth University's School of Pharmacy, who was not involved in the study.
8 Blood Pressure Drugs Linked to Better Memory
ACE inhibitors:
- Captopril (Capoten)
- Fosinopril (Monopril)
- Lisinopril (Prinivil, Zestril)
- Perindopril (Aceon)
- Ramipril (Altace)
- Trandolapril (Mavik)
ARBs:
- Telmisartan (Micardis)
- Candesartan (Atacand)
Source: Hypertension; brand names are listed in parentheses.
Nearly half of adults in the U.S. have high blood pressure, and most take medicine to lower it, federal data shows. High blood pressure is defined as 130/80 millimeters of mercury (mm Hg) or higher, though medication typically isn't recommended until blood pressure reaches 140/90 mm Hg. ACE inhibitors and ARBs are just two classes of pressure-lowering drugs; they work by acting on the body's renin-angiotensin system, which regulates blood pressure.
A handful of medicines in these two classes have properties that enable them to penetrate the brain, where they could have a localized effect, says study coauthor Daniel Nation, an associate professor of psychological science at the University of California, Irvine — especially because in the brain, the renin-angiotensin system “is believed to be involved in functions critical to cognition,” the researchers write.

































































More on health
Easy, Enjoyable Ways to Boost Heart Health and Lower Blood Pressure
How just stretching, taking baths or enjoying your coffee could lower your risk of heart attack and strokeMonitoring Your Blood Pressure at Home
Why it's so important and how to do it right20 Questions to Ask When Dementia is Diagnosed
UCLA experts say information can help patients and families through next steps