Staying Fit
After a brief lull, new cases of COVID-19 are starting to creep back up, both in the U.S. and in Europe, leaving many to wonder whether we’re headed toward a fifth wave, just in time for winter.
The answer, experts say, isn’t as simple as a yes or no. And that’s because we’re in a much different place in the pandemic this year, compared to last.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
“It certainly does feel like a bit of déjà vu, but it’s not the same type of déjà vu,” said Syra Madad, an infectious disease epidemiologist and senior director of the System-wide Special Pathogens Program at New York City Health + Hospitals.
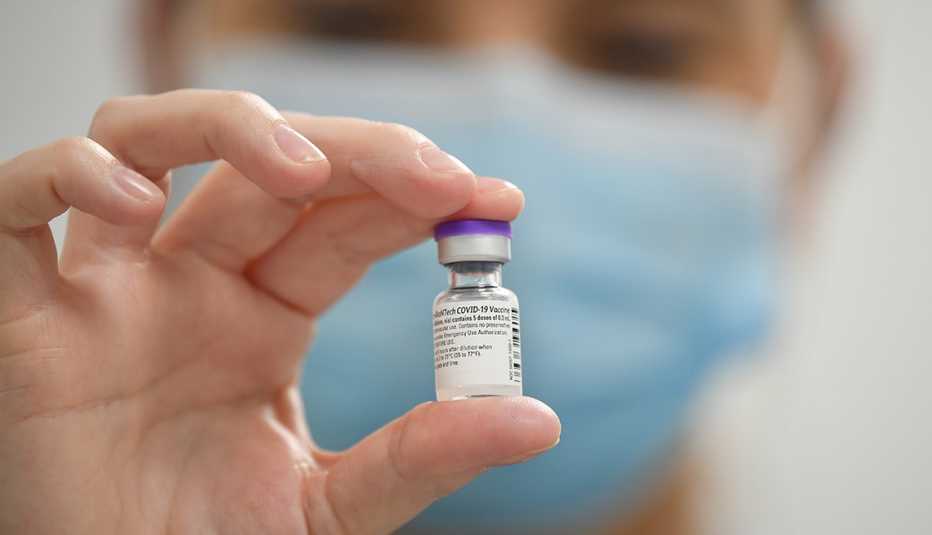
Vaccines will curb infections and illness
For starters, about 60 percent of the U.S. population is fully vaccinated against COVID, meaning nearly 200 million people will be highly protected from hospitalization if they get infected with the coronavirus. Millions of newly eligible kids 5 to 11 will only add to those numbers.
“So even if cases go up this winter, we're very unlikely to see a return to the overcrowded ICUs and makeshift morgues of a year ago,” said David Dowdy, M.D., associate professor of epidemiology at the Johns Hopkins Bloomberg School of Public Health, at a recent media briefing.
Need help getting a COVID-19 vaccine or booster?
Visit vaccines.gov or call 1-800-232-0233 (TTY: 888-720-7489) for assistance in English, Spanish, and many other languages.
Unvaccinated people are over 11 times as likely to die from COVID as vaccinated individuals, recent data from the Centers for Disease Control and Prevention shows. At last winter’s peak, when the vaccines were just rolling out, an average of 3,400 people were dying of the illness each day. Now that average, while still alarming, hovers around 1,000.