Staying Fit

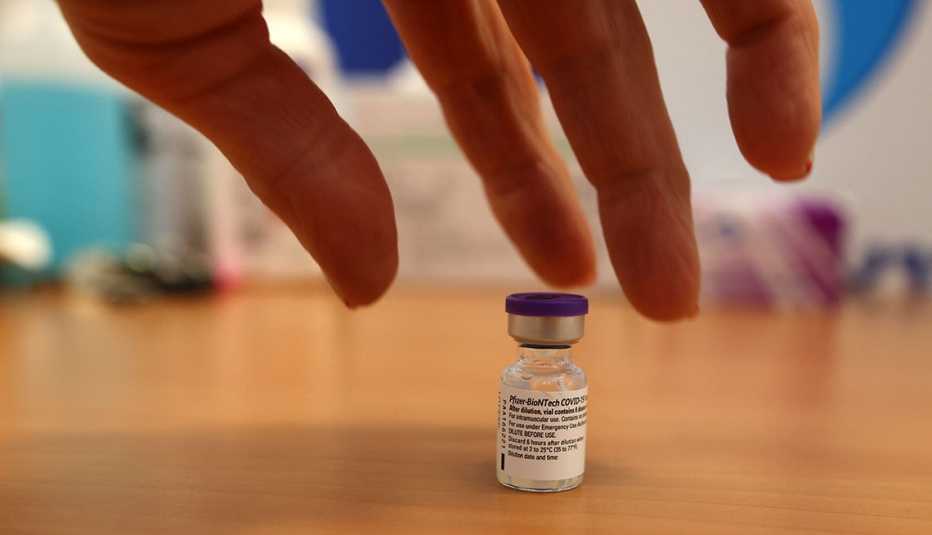
A Centers for Disease Control and Prevention (CDC) advisory panel voted unanimously on Aug. 13 in favor of a decision to allow moderately and severely immunocompromised individuals to receive a third dose of the Pfizer-BioNTech and Moderna coronavirus vaccines. The vote happened one day after the Food and Drug Administration (FDA) expanded the emergency use authorizations (EUA) for the two vaccines.
The change affects a small population whose immune systems are weakened from a solid organ transplant or other conditions that have an equally crippling effect on the immune system — less than 3 percent of American adults, according to CDC Director Rochelle Walensky, M.D., who signed off on the panel’s recommendation hours after the vote.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
“After a thorough review of the available data, the FDA determined that this small, vulnerable group may benefit from a third dose of the Pfizer-BioNTech or Moderna vaccines,” Acting FDA Commissioner Janet Woodcock, M.D., said in a statement. “Today's action allows doctors to boost immunity in certain immunocompromised individuals who need extra protection from COVID-19.”
The Moderately and Severely Immunocompromised
Populations that are considered to be moderately and severely immunocompromised:
- People who have been receiving active cancer treatment for tumors or cancers of the blood.
- People who received an organ transplant and are taking medicine to suppress the immune system.
- People who received a stem cell transplant within the last two years or are taking medicine to suppress the immune system.
- People with a moderate or severe primary immunodeficiency (such as DiGeorge syndrome and Wiskott-Aldrich syndrome).
- People with advanced or untreated HIV infection.
- People undergoing treatment with high-dose corticosteroids or other drugs that may suppress the immune response.
People should talk to their healthcare provider about whether getting an additional dose is appropriate for them, the CDC says.
Source: CDC
Additional shot enhances protection
People who have undergone solid organ transplantation or have other immune-weakening conditions have a reduced ability to fight off infections and are more vulnerable to falling ill from one, the FDA explains. And data presented in the Aug. 13 CDC advisory committee meeting show that a two-dose COVID-19 vaccine regimen is less effective in immunocompromised individuals. This population is also more likely to transmit the virus to household contacts and to get a breakthrough infection that lands them in the hospital.
A third dose of the vaccine, however, could give the immune system the boost it needs to fend off COVID-19, which is a particular concern as the highly contagious delta variant rips through many communities across the country.
A study published this week in The New England Journal of Medicine found that solid organ transplant patients who were given a third vaccine dose saw a significant boost in antibody response against the coronavirus, compared with those given a placebo dose. Some expected side effects were slightly more common in those who received the third dose than in those who received the placebo, however no serious adverse events were reported after the administration of the third dose, the study's researchers write.
The amended EUA allows for the third dose to be administered at least 28 days after completion of the two-dose regimen of the same vaccine to individuals 18 years or older for Moderna, and 12 years or older for Pfizer-BioNTech. It does not apply to the single-shot Johnson & Johnson vaccine, as health officials say there is not enough data to support an additional dose at this time.
A prescription will not be required for immunosuppressed individuals to receive the additional dose, health officials said. If you’re unsure whether a third dose is recommended for you, “send your provider an email or give them a call,” says infectious disease expert William Schaffner, M.D., a professor of medicine at Vanderbilt University School of Medicine.

































































More on Health
10 COVID Vaccine Myths
Fact vs. fiction on the coronavirus shots
4 Reasons You Shouldn't Skip Your Second COVID-19 Shot
Why the final dose of Moderna, Pfizer vaccines could be more important than the firstThe Rising Toll of Autoimmune Diseases in Older People
Why the risk of these common disorders may be much higher than it was for our parents