Staying Fit
It got off to a rocky start — and with ongoing supply shortages, it's still far from perfect. But testing for the new coronavirus is ramping up throughout the U.S., and it's expected to keep expanding.
Here's a look at what's currently available and what's on the horizon for coronavirus testing:
How many different coronavirus tests are out there?
Before the coronavirus started spreading in communities across the U.S., there was just one type of test to detect an infection. This test kit was made by the Centers for Disease Control and Prevention (CDC) and was distributed to a handful of state and local public health labs.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
But since the end of February, more than 25 types of coronavirus tests have come on the market. These have been developed by commercial manufacturers and granted emergency use authorization by the Food and Drug Administration (FDA) — a fast-track approval process of sorts that helps to push out potentially lifesaving tools during a public health emergency.
To date, nearly 1.8 million tests have been used to identify cases of coronavirus in the U.S., according to the COVID Tracking Project. COVID-19 is the disease caused by the new coronavirus.
How do the tests work?
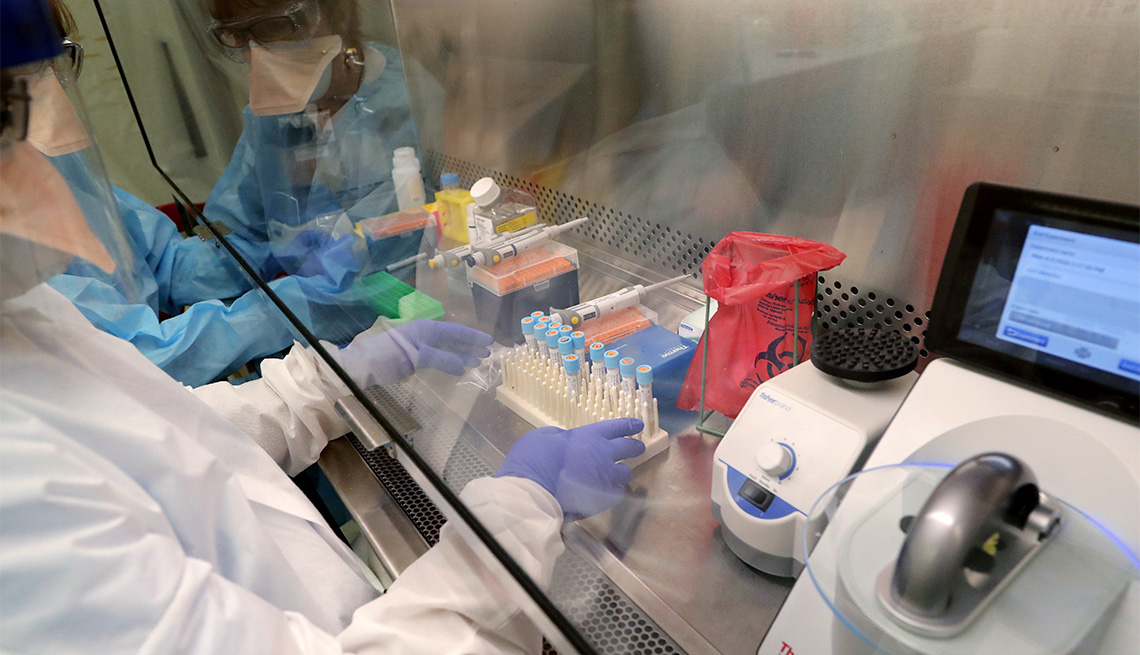
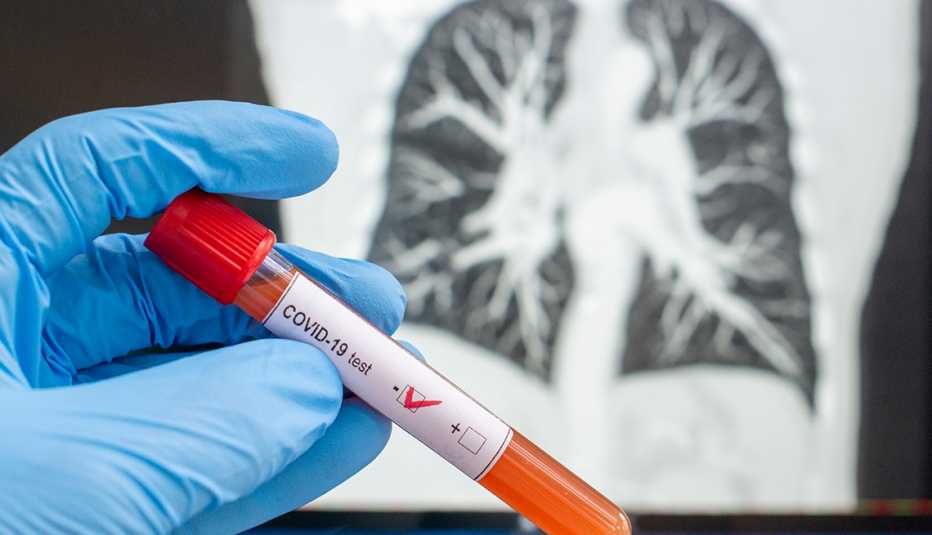
The majority of the available coronavirus tests work similarly: They look for the virus’ genetic material in a sample of mucus, which is usually collected by a nasal or throat swab administered by a health care worker, says pathologist Timothy Stenzel, director of the Office of In Vitro Diagnostics and Radiological Health at the FDA.
One test that has received an emergency use authorization, however, is different: It's a blood test, for starters. And it can tell whether a person had the virus by identifying antibodies, which are basically a signal that the body already responded to an infection.
How long does it take to receive test results?
That depends on a few things. Most of the tests in use are analyzed at off-site laboratories, and results can take anywhere from a day to more than a week to get back to the patient. The major reason for testing delays now is not a lack of testing kits, as was the case at the start of the outbreak. Now the holdup is shortages of the “ingredients” needed to process the tests in the lab, says Eric Blank, chief program officer at the Association of Public Health Laboratories.
"I think the public perception is the swab goes into a black box and then a result pops up. And there's a lot more to it than that,” Blank says.
Reagents, swabs and transport mediums needed for the multistep process are in high demand around the world as the coronavirus continues its spread. “So it's not just a U.S. problem; it's a problem globally. It is getting better, but it's still going to take a while before the pipeline gets filled and we're getting all the supplies we need,” Blank says.