Staying Fit
For Charlene Fugate, 70, of Indianapolis, the trouble started in March with a persistent respiratory infection that required two courses of antibiotics plus an inhaler to help her breathe. After several days, she realized she “was having a harder and harder time” holding her breath for the 10 seconds it took for the steroids to reach her lungs. By the time her husband took her to IU (Indiana University) Health West Hospital, she was also experiencing headaches, fever and coughing.
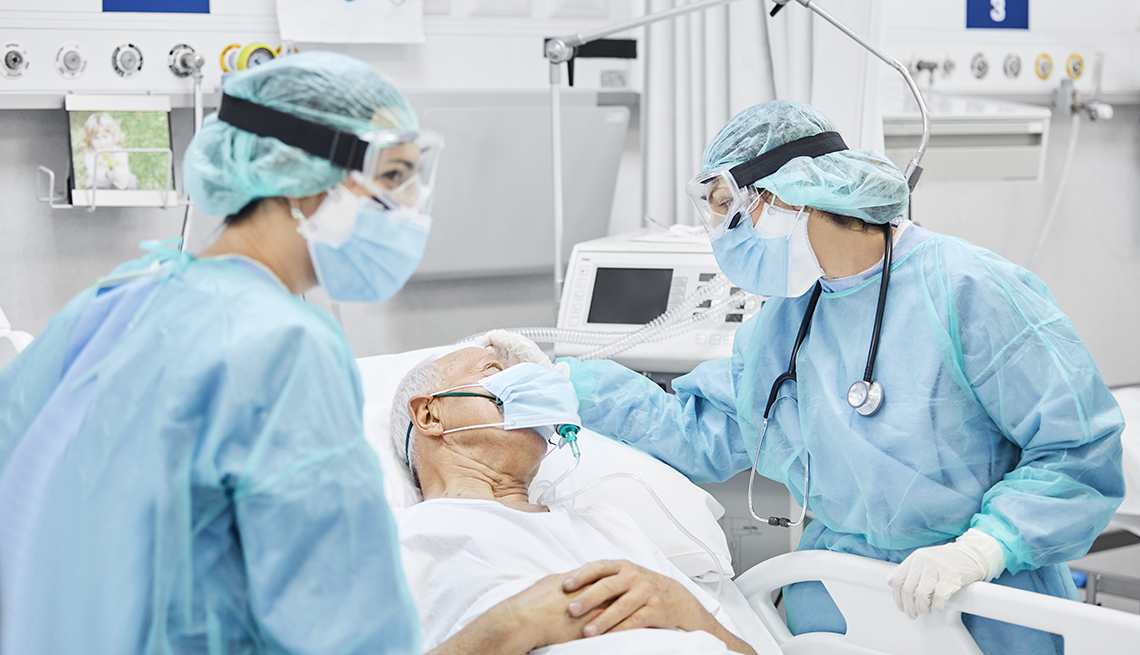
Within 21/2 to three hours of walking into the ER, Fugate was on a ventilator, with an IV, feeding tube and catheter, and was being transferred to the intensive care unit (ICU) at IU Health Methodist Hospital with a diagnosis of COVID-19. She spent three days in the ICU and another four days in a different unit in the hospital before going home. Yet three months later, her recovery is still a work in progress.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
In addition to feeling weak and short of breath at times, Fugate is struggling with getting over what she went through emotionally.
Soon after she left the hospital, Fugate started having flashbacks of her time in the ICU — fragments of memories that she describes as distressing and frightening. And she is haunted by the memory of having to text her family, waiting outside the hospital ER admissions area, to tell them that she was being ventilated, and of worrying she'd never see them again. Not remembering what happened from there also unnerves her. “I lost track of basically three whole days,” she says. “I know that I was taken care of and I had nice nurses, but I really don't know what all happened during those days.”
Though Fugate survived the worst ordeal of her life, she says she also lives with the overwhelming fear that she will get sick again — since no one yet knows whether having COVID confers immunity to the disease. “Leaving the kids and my husband — I'm not ready to do that yet,” says Fugate, who has returned to her job as an accounting coordinator. “I work with a lot of kids — 20- and 30-year-olds — and they seem not to take it as seriously as us older people. Did they social distance? Do they wear their masks outside of here? Do they keep track of their vital signs?"
Fugate is on an antianxiety medication and has talked to a hospital chaplain about her near-death experience. “She told me I'm suffering from a form of grief and a form of PTSD,” she says.
Fugate's story is becoming a familiar one among COVID patients, particularly those who spent time in intensive care. Anyone who has been in the ICU is prone to long-term emotional, cognitive and physical problems, collectively termed post-intensive care syndrome (PICS)—"a very common condition where patients and their caregivers experience quality-of-life impairment for up to two years after surviving critical illness,” says Sikandar H. Khan, an osteopathic doctor, pulmonologist and critical care physician who oversees the Critical Care Recovery Center at IU Health in Indianapolis, one of a growing number of clinics focused on the long-term health problems of ICU patients.