Staying Fit
In a move aimed at saving Medicare money and saving the lives of people with kidney disease, President Trump signed an executive order Wednesday that emphasizes early detection, more patient choice and increased numbers of transplants.
About 1 in 7 adults in the United States have chronic kidney disease, according to the federal Centers for Disease Control and Prevention (CDC). Of the 37 million estimated to have the condition, 9 in 10 don't know it.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
“We aim to reduce the number of Americans developing end-stage renal disease by 25 percent by 2030,” said Alex Azar, secretary of health and human services. “We need to provide patients who have kidney failure with more options for treatment from both today's technologies and future technologies such as artificial kidneys, and make it easier for patients to receive care at home or in other flexible ways."
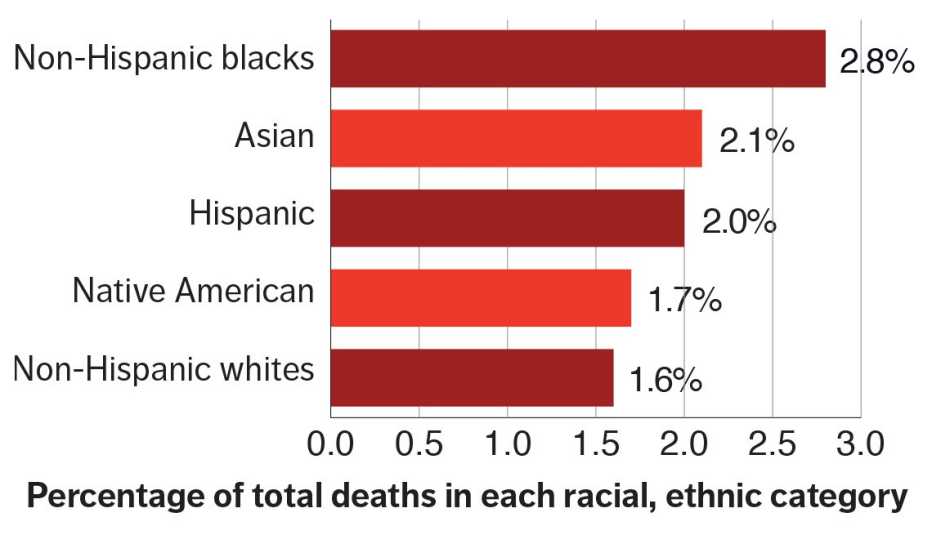
Kidney disease ranked ninth among causes of death in the United States in 2017, the most recent year for which CDC figures are available. Women are more affected than men, and people of African American, Native American, Asian and Hispanic descent die from kidney problems more often than do non-Hispanic whites.

Diabetes and high blood pressure are the two leading causes of kidney failure, the CDC says. The good news: Not all people diagnosed with kidney disease end up in kidney failure. Diagnosing the problem early, controlling the chronic conditions that caused the illness and making healthy lifestyle changes are important to stop the need for dialysis and a new kidney.
“We need awareness, earlier detection and more treatment in a primary setting,” with primary-care physicians overseeing diet and exercise plans to help delay or prevent the need for dialysis, and with patients who need dialysis doing it themselves at home, said Tonya Saffer, vice president of health policy for the National Kidney Foundation.
Part of the intent of Trump's executive order is to launch an awareness campaign that focuses on early diagnosis and incentives for health care providers to keep the disease from progressing to kidney failure.
Kidney disease coverage under Medicare
Since 1972, Medicare has covered people of any age diagnosed with permanent kidney failure that requires dialysis or a kidney transplant, called end-stage renal disease. A diagnosis of end-stage kidney failure usually happens when a patient has just 10 to 15 percent of kidney function remaining, according to the National Kidney Foundation.
The government-funded health care plan also covers those age 65 and older who have chronic kidney disease, lasting damage to the kidneys that can get worse over time.