Staying Fit
Eczema — that itchy, angry red rash that plagued your childhood — is often dismissed as a children's disease. But almost 10 percent of all adults suffer from this condition, as well. And though the prevalence of eczema dips in young adulthood and middle age, it surges again in adults over 74, according to a study published recently in the Annals of Internal Medicine. “People's skin gets drier as they age, so often someone who had eczema in childhood sees it disappear in adulthood, only to reappear once they hit their 60s or 70s,” explains Lawrence Eichenfield, M.D., chief of Pediatric and Adolescent Dermatology at the University of California San Diego School of Medicine. Here's everything you need to know about this disease: what it is, how to treat it and how to prevent it from driving you nuts.
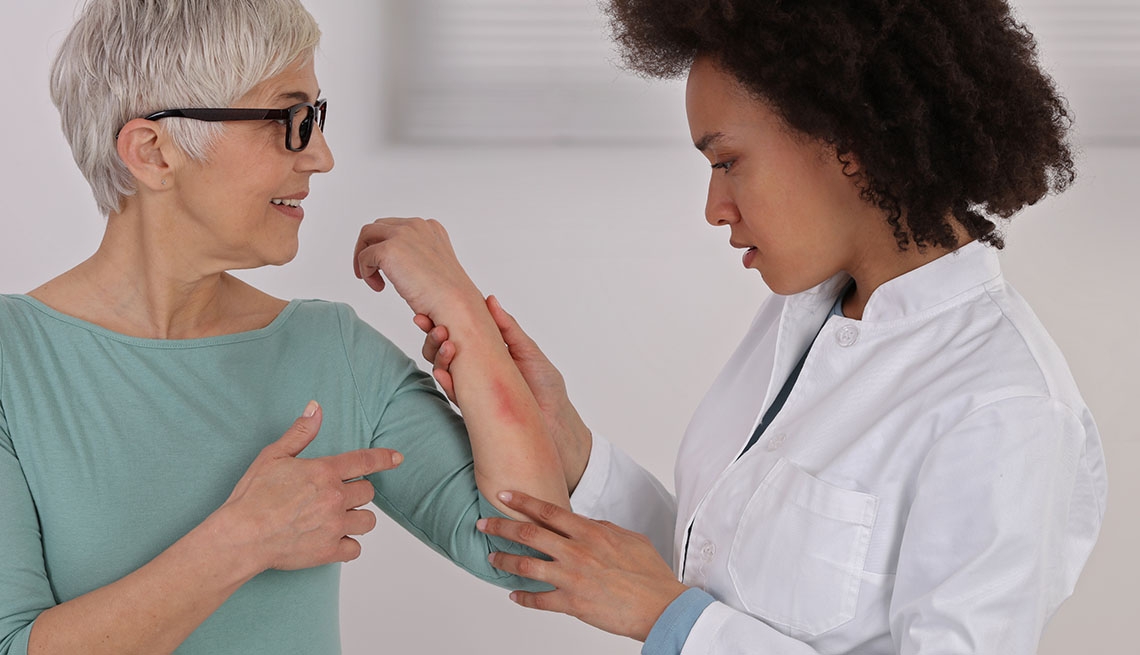
At any age, eczema is itchy


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
Unlike kids, who tend to get the condition on places like their cheeks or scalp, adults are most likely to find it in nooks and crannies, including on the backs of their knees and elbow crooks, and even around their eyes. But the same as when you were a kid, eczema tends to be very, very itchy. “It can affect an adult's quality of life just as much as it affects a child's — causing sleep loss, depression, anxiety and even an increased risk of skin infection,” Eichenfield explains.
Eczema flare-ups can be triggered by something known as the “itch-scratch cycle,” Eichenfield says. This is when itching leads to scratching, which results in the release of inflammatory chemicals that worsen eczema by drying out the skin. The vicious cycle continues unless you step in and treat the disease.