Staying Fit

If you live long enough, you’ll probably get cataracts, which are an inevitable consequence of getting older. The eye lens can begin to cloud in middle age and by 80, more than half of all Americans will either have cataracts or have had cataract surgery. “I liken cataracts to wrinkles and gray hair,” says Anupama Horne, an ophthalmologist and eye surgeon at Duke University in Durham, N.C. In the end, nearly everyone will develop them.
But the good news is that today’s high-tech procedures restore clear vision in 90 percent of the 3 million Americans who undergo cataract surgery every year.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
What they are
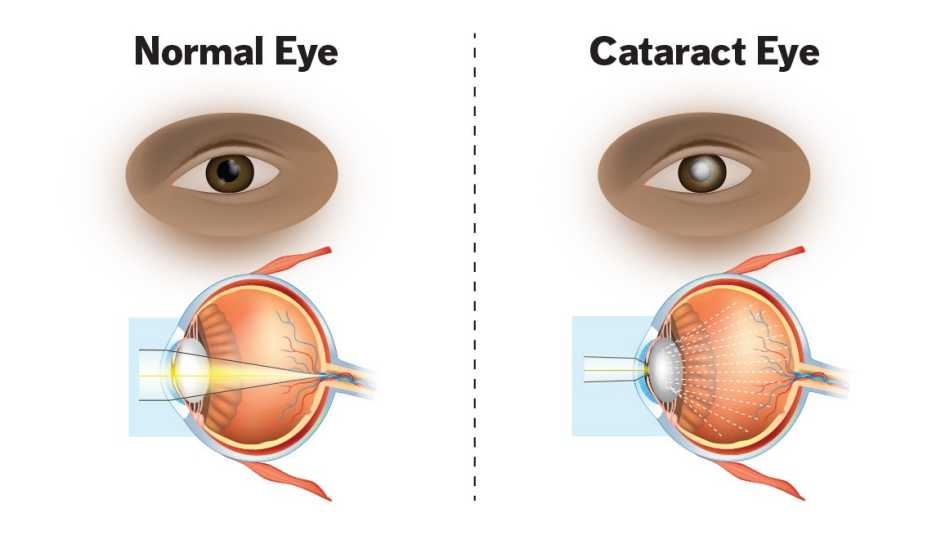
Cataracts usually occur when normal proteins in the lens of the eye break down, causing the lenses to become cloudy. The lens of the eye works much like a camera's: It focuses light onto the retina at the back of the eye, which then relays nerve signals to the brain, and it adjusts the eye’s focus, enabling us to see things clearly up close and far away. But the normal wear and tear of aging causes the proteins to clump together, which clouds the lens, gradually making it harder to see as the cataract grows larger. Cataracts usually take a long time to develop, and can occur in one or both eyes but won't spread like an infection from one eye to the other.

Causes
Aging is the most common cause of cataracts, but other culprits can contribute, including certain medications, chronic illnesses, poor health habits or too much sun without protection. “Being extremely near-sighted is also associated with a higher frequency of cataracts,” says John D. Dugan Jr., an ophthalmologist and cataract surgeon at the Wills Eye Hospital in Philadelphia. “But we’re not sure why.” Family history plays a role, too.
Symptoms


Because age-related cataracts generally develop over time, gradually worsening vision may not be noticeable. But as the clear lens of the eye slowly turns a yellowish/brownish color, the increased tinting may make it more difficult to read and colors seem faded. Other symptoms include blurry or double vision, glare — when headlights, lamps or sunlight appear blindingly bright — and poor night vision that can make driving hazardous.
“It’s like a piece of clear plastic becomes yellowed and discolored,” says John Bartlett, an ophthalmologist and eye surgeon at UCLA Stein Eye Institute in Los Angeles. “As new layers are added, it becomes denser and harder.”


































































More on health
Get the Facts on Glaucoma
Early diagnosis and treatment can lower your risk of vision lossThe 10 Best Superfoods for Your Eyes
Protect your vision with these nutritious (and delicious) foods