Staying Fit


More than 300,000 Americans die each year from sudden cardiac arrest outside of hospitals, but many of them could be saved by everyday heroes such as you.
Cities across the U.S., including Pittsburgh, Seattle and San Diego, are installing automated external defibrillators (AEDs) in public places such as government buildings and schools, as well as in fitness centers, large apartment buildings and dental offices. These devices, found in wall cabinets just like fire extinguishers, can shock the heart and literally bring a person back to life — not unlike a dramatic moment on a hospital TV show. (“Clear!”) The problem with waiting until medical help arrives is that every minute of delay lowers the chance of survival by 7 to 10 percent, according to an American Heart Association report.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
Use of AEDs by bystanders doubled from 2006 to 2015, but it’s still relatively uncommon. In only 6.7 percent of cases did someone other than emergency personnel administer aid. Often, people who see someone in need won’t use an AED because they don’t think they can operate it. That’s an unfounded fear, according to Clifton Callaway, professor of emergency medicine at the University of Pittsburgh and chair of the American Heart Association’s Emergency Cardiovascular Care Committee. The device is automatic, he says, and “a 911 operator can talk you through it.”

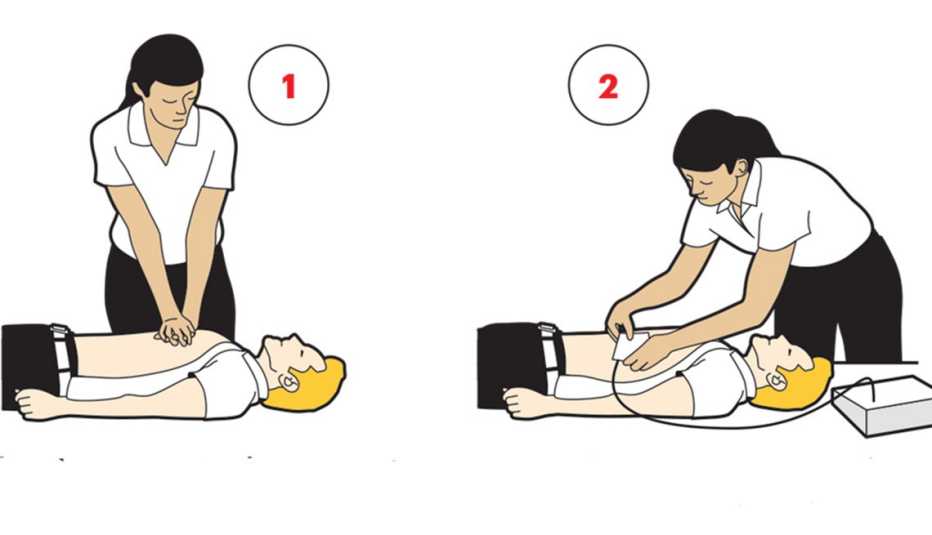

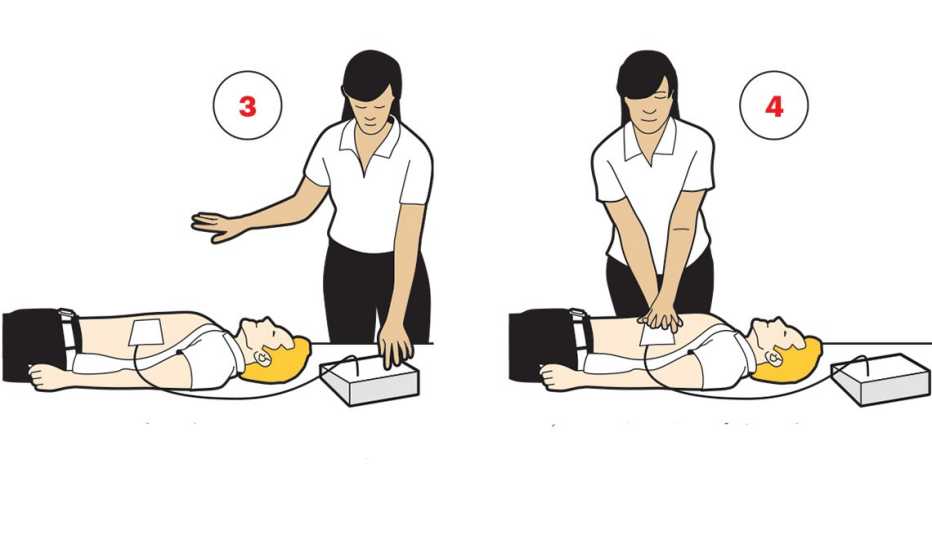
Studies have indicated how simple AEDs are to operate. In one, published in the journal Circulation, sixth graders using AEDs on mannequins were able to defibrillate a victim’s heart in about 90 seconds — not vastly different from the time of 67 seconds achieved by emergency medical technicians.
Laws regulating who may use AEDs vary by state, but most states have Good Samaritan laws that protect from liability anyone using an AED in an emergency, according to the National Conference of State Legislatures.
“Only 15 states and the District of Columbia require an AED in a health club or gym, and just 17 states require one in schools. Meanwhile, the nonprofit PulsePoint Foundation has developed an app that allows emergency personnel and citizens to quickly locate the nearest AED. The free app also allows the community to report AED locations to build a more comprehensive AED registry.”


Reality Star's Life Saved by AED
Feb. 12 was a day that Bob Harper can’t remember but will never forget. During a workout the 52-year-old fitness expert and former cohost of NBC’s The Biggest Loser started feeling dizzy and lay on the ground. A fitness coach at the gym called 911 and performed CPR. Harper turned blue. Two doctors who were there used an AED to shock Harper back to life. He woke in a hospital two days later and was told he had suffered cardiac arrest.
“When I was on the ground, I was already dead,” he says. Today, Harper has two stents in his arteries, an even healthier lifestyle and an appreciation for AEDs. “Life can turn on a dime,” he says. “I believe that AEDs should not only be in gyms but in restaurants, airports and everywhere people congregate.”

































































More From AARP
Simulation Shows Promise for Drone Use in Cardiac Arrest
Unmanned aircraft could deliver a defibrillator much faster than ambulances