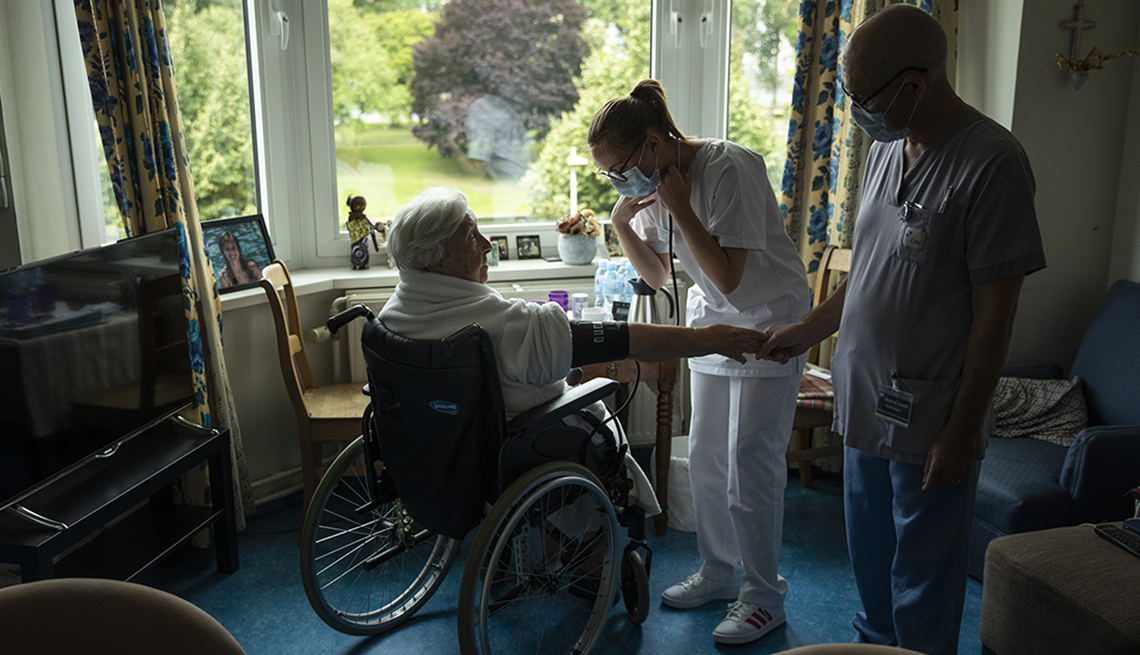Staying Fit
Nursing homes continue to be hot spots for COVID-19, especially as cases increase in the South and West.
Both residents and staff are at high risk for infection and death. Even now, 44 percent of all virus-caused deaths, or more than 56,000 deaths in all, have occurred in long-term care facilities, according to a July 13 report from the nonprofit Kaiser Family Foundation. And that doesn't account for four states — Alaska, Hawaii, Montana and South Dakota — that haven't reported nursing home deaths.


AARP Membership— $12 for your first year when you sign up for Automatic Renewal
Get instant access to members-only products and hundreds of discounts, a free second membership, and a subscription to AARP the Magazine.
But a full-scale “second wave” could arrive as early as mid-September, a specter that is troubling to experts and advocates. They urge that steps be taken now to curb the number of future deaths, and in interviews they recommend seven staffing policies that they say could protect residents and staff.


Doctor: Hospitals, nursing homes face similar problems
As COVID-19 swept across New England, Sunil Parikh, M.D., has played a rare dual role in aiding both the ailing residents and worried managers of Connecticut's nursing homes.
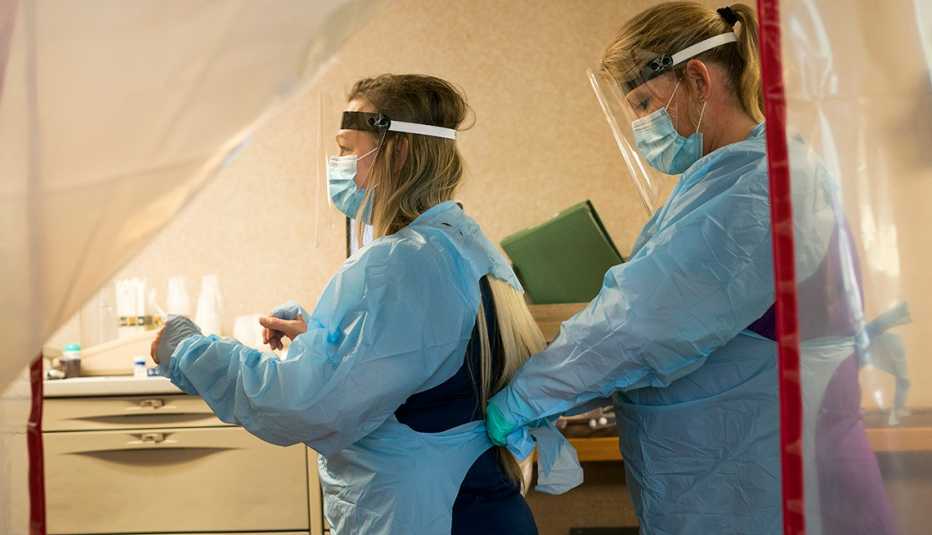
Parikh, an infectious diseases physician at the Yale School of Medicine, helped colleagues at Yale New Haven Hospital review the cases of a flood of patients from nursing homes. Then he became part of the weekly calls state health officials led, counseling facilities on navigating COVID-19. He noticed that both his hospital and nursing homes faced similar challenges, such as shortages of masks and gowns.
"But there was this disconnect between the two groups,” said Parikh, also an associate professor of epidemiology at the Yale School of Public Health. If the nursing homes had sufficient testing, gear and other tools, they could keep more residents healthy and ease the crush on overburdened hospitals, he concluded.
Nursing homes need to be able to test all residents and staff even if they aren't showing symptoms. That would be expensive, and Parikh said state and federal governments likely would have to share the cost.
"I feel this aggressive approach is needed given how explosive and devastating COVID-19 can be in these settings,” he says. “The downstream effects would be huge."
"There are certain things that would cost more to do, but the real cost is loss of life for the failure to do things,” says Elaine Ryan, AARP vice president for state advocacy and strategy integration. AARP is urging Congress to require COVID-19 testing of staff and residents, provide personal protective equipment (PPE) to staff and have enough staff to meet residents’ needs.
Several sources mentioned the story of a small assisted living facility in Bristol, Connecticut. In mid-March, Tyson Belanger, owner of Shady Oaks Assisted Living, brought 22 staff members to live on-site full time to prevent them from carrying in the virus as they went about their lives in the community between Hartford and Waterbury.
The last live-in staff members left after 70 days, and the home had no coronavirus cases, he said in a telephone interview. As of July 7, the facility continued to have no cases, according to a report from the Connecticut Department of Public Health.
This won't work for most places — Belanger spent about $250,000 of his own money on payroll and supplies — but Belanger's experience shows how employees play a key role in the health of residents in long-term care. To date, 1,071 cases and 371 deaths have been reported among Connecticut assisted living residents; 8,850 cases and 2,755 deaths among the state's nursing home patients.